Digest This
Click on the topics below to learn how probiotics can improve your digestive health, naturally.
The IBS/Traveler’s Diarrhea Connection
- @drHoberman
- Digestive Health
The holiday travel season may be long over, but the memories of that special trip, maybe to a warmer destination many time zones and thousands of miles away, still resonates.
Your only sour memory of that trip is a bad case of traveler’s diarrhea, the most common ailment vacationers face when they journey long distances, particularly to international destinations like South America, Africa, Mexico and Asia.
That run-in with traveler’s diarrhea could leave you vulnerable to irritable bowel syndrome (IBS), the most common gut health problem that affects up to 15 percent of all Americans, according to the American College of Gastroenterology.
A weakened immune system
Although researchers are still trying to figure out all of the answers, a recent study may have found an important connection between IBS and traveler’s diarrhea, according to a recent study appearing in the journal Cell.
To support a healthy gut, our body’s immune system must be equipped to maintain a balanced response to problems as they come without overdoing it.
For example, inflammation can help the gut fight an infection, but too much of a response “can cause lasting harm,” says Dr. Daniel Mucida, head of The Rockefeller University’s Laboratory of Mucosal Immunology.
After Dr. Mucida and his team treated mice with a weak form of Salmonella (a very common bacterium that causes food poisoning), they discovered a lingering drop of neurons in the gut that could create an inflammatory response.
Previous work by Dr. Mucida determined these neurons could also be triggering the death of a specialized set of gut immune cells that can lead to constipation, a key IBS symptom.
A gut bacteria imbalance
Not surprisingly, this research team also discovered treating mice with Salmonella tipped the balance of beneficial gut bacteria in their tiny bodies in a bad way.
However, those neurons recovered when scientists restored the healthy balance of bacteria in those very same mice.
Fortunately, one of critical steps you should take to prevent traveler’s diarrhea — taking a probiotic — works very well when treating IBS too.
That being said, not just any kind of probiotic will do the trick.
Many probiotics are formulated with a single strain of bacteria to treat a specific problem, but not the kinds that patients encounter with IBS.
Based on a very recent review in the journal Nutrients, patients experienced greater benefits when taking probiotics with multiple strains of beneficial bacteria for at least eight weeks.
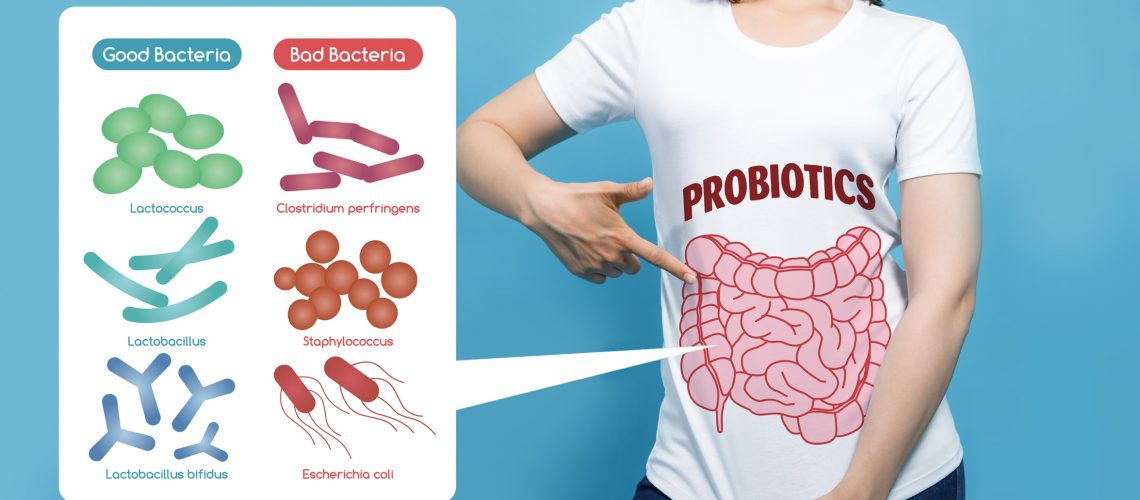
The human gut is populated by more than 1,000 species of bacteria. A probiotic made with multiple strains of beneficial bacteria is formulated to boost your immune system and treat IBS more effectively.
Taking a product like EndoMune Advanced Probiotic made from 10 strains of beneficial bacteria from the Lactobacillus and Bifidobacterium families plus a prebiotic (FOS) that feeds the good bugs in your gut may be the safer and more effective choice for treating IBS and traveler’s diarrhea too.
References
There Is An Endomune Probiotic For Every Lifestyle
-
EndoMune Metabolic Rescue
$44.95 -
EndoMune Advanced Probiotic
$42.95 -
EndoMune Companion Pack
$112.93