During winter months, we see more colds, more missed days of work and school, and more families looking for natural immune support. In one large clinical trial, people taking a specific probiotic mix had cold season symptoms on only 4.5% of study days compared with 6.7% for placebo, a relative reduction of about one-third in the time they felt sick.
Key Takeaways
Question | Answer |
| How do probiotics help immunity during cold season? | They support gut health, where most of the immune system resides, helping balance good bacteria and modulate immune responses. Learn more in our article on the gut–immune system connection. |
| Can probiotics shorten colds? | Clinical trials show certain probiotic blends can reduce how many days people experience cold symptoms and may lessen severity. |
| Which probiotic is best for general immune support? | A multi-strain, high CFU formula with a prebiotic, such as EndoMune Advanced Probiotic, provides broad support for gut and immune health. |
| What about children’s immunity during winter? | Kid-specific probiotics can support digestive and immune health. Explore child-focused options in our Children’s Health category. |
| Are infant probiotics useful for early immune support? | Gentle infant probiotics help establish a healthy gut, which naturally supports developing immunity. Learn more in our article on probiotics for preterm and newborn babies. |
| Where can I view all EndoMune probiotic supplements? | You can see our full line of gut and immune support formulas in the Shop Probiotics section. |
1. Why Cold Season Challenges Your Immune System
Cold season brings together several stressors on your immune system, including more time indoors, drier air, and greater exposure to respiratory viruses. At the same time, holiday eating patterns, travel, and higher stress can disrupt the gut, which is home to much of the body’s immune activity.
When gut balance shifts, the immune system can become less efficient at recognizing and responding to everyday threats. We see this play out as more frequent colds, longer symptom duration, and slower recovery, especially in families juggling work, school, and childcare.
The Gut–Immune Connection In Winter
Research has linked specific gut microbes to upper respiratory tract infection risk, which reinforces how closely the gut and respiratory immune systems communicate. During cold months, supporting a healthy gut environment helps maintain this communication so immune cells respond quickly and appropriately.
This is where a well-formulated probiotic supplement can be a practical daily tool. By providing beneficial bacteria and, in some cases, prebiotic fibers, probiotics help maintain a resilient gut environment that supports immune defenses when exposure risk is highest.
2. How Probiotics Help Your Immune System Fight Colds
Probiotics support immunity during cold season in several complementary ways. They help crowd out potentially harmful bacteria in the gut, support the gut barrier, and influence immune cell activity.
In practical terms, this can mean fewer days with symptoms, less severe congestion or sore throat, and a quicker return to normal routines. Clinical studies in adults and children show that targeted probiotics can shorten the duration of cold and flu-like symptoms and reduce the need for medications like fever reducers.
Key Gut–Immune Actions Of Probiotics
- Support the balance of beneficial bacteria, which helps keep the gut lining healthy.
- Interact with immune cells in the intestinal wall, helping regulate inflammation.
- Encourage production of antibodies, including IgA, that protect mucosal surfaces like the nose and throat.
- Help the body respond more effectively to everyday viral exposures during winter.
Because 70 percent or more of the immune system is associated with the gut, this kind of daily support can make a meaningful difference in how you experience cold season. That is why many of our customers use a daily probiotic as part of their core wellness routine alongside sleep, nutrition, and hygiene.
3. Science Spotlight: What Clinical Trials Show About Probiotics And Colds
Several well-designed human studies have examined how probiotics impact respiratory infections and cold symptoms. In adults, one randomized controlled trial found that a specific probiotic mix cut the proportion of days with cold symptoms by about one-third compared to placebo.
In children, another trial showed that those receiving a probiotic had fevers that lasted about 2 days less than the placebo group during upper respiratory infections. Shorter fever duration means fewer missed school days and less stress for parents.
What This Means For Real Life
These trials do not mean that probiotics completely prevent every cold, and no supplement can promise that. What they suggest is that when illness does occur, a healthy gut supported by probiotics may help you and your family feel better sooner and with less intensity.
When we design an advanced probiotic supplement, we look closely at this kind of data, focusing on multi-strain formulas and adequate CFU counts that align with what has been studied in humans during cold and flu seasons.
Did you know?
In children with upper respiratory tract infections, fever duration was about 2 days shorter (median 3 days vs 5 days) when they received a probiotic compared with placebo.
4. EndoMune Advanced Probiotic: Daily Gut And Immune Support For Adults

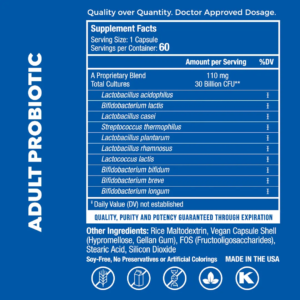
For adults looking for daily support during cold season, EndoMune Advanced Probiotic is our flagship formula. It contains a synbiotic blend of 10 beneficial strains and a prebiotic to promote the growth of healthy bacteria in the gut.
Each delayed-release vegan capsule delivers 30 billion CFUs, designed to survive stomach acid and reach the intestines where they can offer the most benefit. At $42.95 per bottle, it provides a month of once-daily support for gut and immune health.
Why We Formulated This Advanced Probiotic
- Developed by a practicing board-certified gastroenterologist who has seen firsthand how gut health impacts immunity.
- Includes the prebiotic fructooligosaccharides (FOS) to nourish beneficial bacteria already living in your gut.
- Supports digestive comfort while helping maintain a robust immune system, particularly helpful during winter.
You can take one capsule daily with or without food, and if you prefer, you can open the capsule and sprinkle it on soft food or mix it into a smoothie. This flexibility makes it easier to stay consistent, which is important when you want steady support across the entire cold season.

This infographic explains five ways probiotics support immunity during the cold season.
Learn practical steps to include probiotic-rich foods in your routine.
5. Supporting Metabolic And Immune Health Together With EndoMune Metabolic Rescue

Cold season often coincides with changes in eating patterns, weight gain, and higher blood sugar swings, all of which can affect immune resilience. EndoMune Metabolic Rescue is a
carefully formulated prebiotic and probiotic combination designed to support metabolic efficiency while still offering all-natural gut support.
This advanced formula helps maintain healthy blood sugar and cholesterol levels while supporting regularity and overall digestive comfort. Better metabolic health can work hand in hand with a healthy immune system, particularly during the winter months when lifestyle habits sometimes shift.
How This Probiotic Supplement Fits A Winter Routine
- Provides a blend of targeted strains plus prebiotics to support gut metabolism and beneficial bacteria.
- Daily dosage is four capsules, taken as two capsules twice per day, which you can coordinate with meals.
- At $44.95 per bottle, it offers an option for adults who want gut and metabolic support together during cold season.
Many of our patients and customers like to pair a metabolic-focused probiotic with lifestyle steps like consistent movement and balanced meals. Together, these choices can help keep energy and immunity steadier through the darker, colder months.
6. Immune Support For The Youngest: EndoMune Baby Probiotic Powder
Infants and toddlers face their own set of cold season challenges as their immune systems learn to recognize new viruses. A healthy gut is crucial during this time because it helps train the immune system while supporting comfortable digestion.
learn to recognize new viruses. A healthy gut is crucial during this time because it helps train the immune system while supporting comfortable digestion.
EndoMune Baby Probiotic Powder is a gentle probiotic supplement for newborns to age 3, including those delivered by Caesarean section or those who struggle with infantile colic. Each serving provides 10 billion CFUs with a prebiotic to foster a healthy gut environment.
How This Infant Probiotic Supports Immunity
- Promotes digestive health, which naturally supports immune development in early life.
- Includes a prebiotic to help beneficial bacteria thrive, particularly important in babies with early antibiotic exposure.
- Easy to use: simply mix one scoop into breast milk, formula, or soft food once daily.
At $29.95 per bottle, this powder provides a month of infant-friendly gut and immune support. For families wanting to stay prepared through cold season, the EndoMune Baby Powder Twin Pack offers 10 percent savings at $53.91.
7. Kid-Friendly Immunity: EndoMune Kids Advanced Chewables
School-age children encounter many respiratory viruses during fall and winter, from classroom exposures to sports and playdates. Supporting their gut health with a child-focused probiotic can help keep their digestive and immune systems resilient.
EndoMune Kids Advanced Chewable Probiotic delivers 10 billion CFUs per tablet in a sugar-free, kid-approved chewable. The EndoMune Kids Chewable Twin Pack, priced at $59.31, is ideal for families who want an ample supply through the season.
How Our Kids Probiotic Fits Daily Routines
- Children ages 3 to 8 can chew one tablet daily, which fits easily into breakfast or bedtime routines.
- We recommend taking it two hours before or after antibiotics if your child needs those medications.
- The blend includes both probiotics and prebiotics to help maintain a healthy balance of gut bacteria that supports immune function.
For families who want to try the formula first, our EndoMune Kids Advanced Chewable Probiotic Trial is available for $0.00, with a small shipping and handling fee. This lets you see how your child tolerates a probiotic supplement before committing to a full-size bottle.
Did You Know?
Genetic research has identified dozens of gut microbes associated with acute upper respiratory infections, underscoring how closely gut balance and cold risk are linked.
8. Building A Family Probiotic Plan For Cold Season
Many households want a coordinated approach, so every family member receives age-appropriate gut and immune support. That is why we created options that cover infants, children, and adults with consistent quality standards and similar usage patterns.
For example, parents may choose EndoMune Advanced Probiotic for themselves, EndoMune Kids Chewables for school-age children, and EndoMune Baby Probiotic Powder for the youngest family members. This creates a simple, daily routine that supports the gut health of the entire household through the winter months.
Comparing Key EndoMune Probiotic Options
Our EndoMune Family Pack, listed at $101.02, provides a convenient way to support adults and children together with a bundled option. For families that anticipate a busy winter with school and travel, having these probiotic supplements on hand can help you stay ready.
9. Practical Tips: Getting The Most From Probiotics During Cold Season
A probiotic supplement works best when it is part of a consistent, daily routine. We generally recommend taking your chosen EndoMune probiotic at the same time each day, such as with breakfast, to support steady gut health across the season.
If you or your child are taking antibiotics, separate the probiotic by at least two hours to support better survival of the beneficial bacteria. Continue using the probiotic for several weeks after the antibiotic course ends to help restore balance.
Other Habits That Work With Probiotics
- Focus on whole foods with fiber, which act as natural prebiotics for your gut bacteria.
- Practice regular handwashing and adequate sleep, since these are fundamental to immune strength.
- Stay hydrated, especially in dry, heated indoor environments, to keep mucosal barriers healthy.
When these everyday steps are paired with an advanced probiotic supplement that supports gut health, you provide your body with multiple layers of defense during cold season. This comprehensive approach is what we encourage in our practice and in our product development.
10. Frequently Asked Questions About Probiotics And Winter Immunity
We often hear similar questions from patients and customers when they start thinking about probiotics for cold season. Clear answers help you decide how a gut health supplement can fit into your own plan.
How Long Should I Take A Probiotic Before Cold Season?
We typically suggest beginning at least a few weeks before peak cold and flu activity, and then continuing throughout winter. This gives your gut time to adjust and allows beneficial bacteria to establish a stable presence.
Can I Keep Taking Probiotics All Year?
Yes, many people safely use probiotics year-round to support ongoing gut and immune health. If you have specific medical conditions or concerns, discuss long-term use with your healthcare provider.
Do Probiotics Replace Flu Vaccination Or Other Medical Care?
No, probiotics are not a substitute for recommended vaccines or professional medical evaluation. We see them as one part of a comprehensive approach that includes vaccines, healthy lifestyle choices, and prompt medical care for concerning symptoms.
Conclusion
Cold season puts real pressure on your immune system, and supporting your gut is one of the most practical ways to strengthen your defenses. Clinical research shows that targeted probiotics can shorten the duration and reduce the severity of colds in both adults and children.
By choosing a high quality, multi-strain probiotic supplement like EndoMune Advanced Probiotic for adults, and our pediatric and infant formulas for younger family members, you give your gut and immune system daily support when it matters most. Combined with healthy lifestyle habits, probiotics offer a natural, science-backed way to navigate winter with greater resilience and comfort.






 The term “synbiotic” refers to a combination of probiotics and prebiotics working together as a system. Probiotics are the live beneficial bacteria; prebiotics are the non-digestible fibers that feed those bacteria and help them thrive in the gut environment.
The term “synbiotic” refers to a combination of probiotics and prebiotics working together as a system. Probiotics are the live beneficial bacteria; prebiotics are the non-digestible fibers that feed those bacteria and help them thrive in the gut environment.










